
Financial challenges facing the NHS
PiHealth tool enhances NHS invoice validation, boosts efficiency and accuracy.
Our Client.

How to fully understand the costs of the NHS
Since the NHS was founded in 1948, its spending has increased annually by 4% on average in real terms. Its budget, however, has not increased in line with this. At the same time, demand for NHS services has continued to rise due to population growth, longer life expectancies, more complex illnesses arising and more treatments becoming available. As a result, the quality and standards of NHS services have fallen, with waiting times for A and E, hospital appointments, and treatments growing every year.
The demand for NHS services has skyrocketed in 2020, driven by the emergence of Covid-19. Fortunately, the Chancellor has significantly expanded the NHS budget to support efforts to tackle the virus, stating “whatever extra resources the NHS needs, it will get”. While this move has been welcomed by the nation, the funds injected into the NHS do not even meet the threshold needed to balance NHS spending. Unfortunately, these short-term funds will not remedy the long-term financial complications that the NHS has been struggling with for years.
The blueprint for survival
To prevent the quality of services from falling further, the NHS regrettably cannot rely on their budget increasing. They instead need to focus on improving the ‘health value’ they can offer to patients. This means maximising the health outcomes of their patients while minimising costs; working smarter instead of harder. The methods of running the NHS need to be re-evaluated, adapted, and even transformed to create a more efficient service.
To start making changes, it is critical to fully understand the costs of the NHS. This information encompasses the funding designated to NHS activities, the price breakdown of those activities, the reasons behind those prices, and the economic outcomes of those activities.
It is of great concern then, that upon evaluating NHS bodies only a limited number of organisations were found to regularly use cost data outside of the finance department. Further, cost information was used even less by clinicians to improve the efficiency of their services. Without clarity and transparency over the cost data of NHS activities, it is impossible to determine how the economic outcomes of those activities can be improved.
Our client
Pulse Informatics is a healthcare analytics company offering consultancy services to NHS organisations. They strive to enhance the work of Clinical Commissioning Groups, Clusters, and GPs by supporting them with business intelligence, analytics solutions, and data warehousing. By providing better analytics, Pulse Informatics hopes to make decision-making among NHS organisations more informed and effective; saving the NHS money, time and supporting them to more effectively meet patient expectations.
Our target area
To support the NHS in more accurately tracking their cost data, Pulse Informatics sought to target their support towards the needs of NHS Commissioners. Commissioners are needed to plan, agree and monitor NHS services. They include GPs, Clusters, or Commissioning Groups. They play a key role in working towards the NHS Triple Aim of improving population health, quality of care, and cost-control.
Pulse Informatics wanted to tailor its support around the role of commissioners to monitor the efficiency of services more effectively. They decided to do this by maximising their potential savings through invoice validation. Invoice validation in the NHS is necessary for NHS providers to be paid. Providers are required to send invoices to the commissioners of their service for payment. Commissioners then need to accept or challenge the ‘activity’ that is billed to them. This activity includes any type of care that a patient receives. Pulse Informatics wanted to create a tool for commissioning groups to make the invoice validation process a more efficient and less labor-intensive process, with a higher chance of accuracy and a reduced chance of error. They approached us to support them in transforming their vision into a reality.
Our starting point
Before developing the invoice validation tool, commissioning groups would implement a range of software and tools to generate, send and resolve challenges. For instance, users might write up challenge queries in a database. Query results might then be displayed in a spreadsheet. Challenges would then be emailed to the provider. This could then trigger a back-and-forth process of challenges and counter-challenges.
The traditional method of invoice validation is therefore a labor-intensive task. Information is input from a variety of analysts and is displayed and exchanged using a variety of applications and software.
Our solution: PiHealth
At the beginning of our partnership with Pulse Informatics, we held in-depth discussions about their vision for the project and their needs. Based on these discussions, we knew that all information and exchanges involved in the invoice validation process would have to be centralised. We planned to achieve this by designing software that would deal with every stage of the process. This would make information more accessible, and easier to locate and review. This would also reduce the chance of information getting lost or duplicated along the way. Additionally, we wanted to reduce the labour intensity of this process by introducing a means of automating all tasks involved in the process.
When challenges are sent to a provider, our PiHealth tool allows Commissioners to:
- Assign challenges to a provider.
- Maintain provider contact details.
- Indicate whether a provider should be challenged.
- Initiate, schedule, or reschedule challenges.
- Re-run challenges for single or multiple providers.
- Send (via email) single or multiple challenges to providers.
- Send a recall email to invalidate a previous email.
- Download challenge emails & challenges for all providers.
- Agree, disagree, or counter-challenge provider responses.
- Add comments to challenge emails and challenges.
- Track the current status of a challenge and indicate which party the pending action rests upon
- View daily notifications that summarise provider responses.
- View and download previous months’ challenge emails and challenges that were either won, lost, or disputed.
- View challenge timetables for all providers.
- Retrieve SLAM reports that providers have uploaded to a SLAM report repository.
Our tool also allows providers to:
- View and download their challenges from all commissioners.
- Accept, accept with an adjusted value or reject challenges.
- Add comments to challenges.
- Track the current status of a challenge and indicate which party the pending action rests upon.
- View daily notifications that summarise commissioner responses.
- View and download previous months’ challenge emails and challenges that were either won, lost, or disputed.
- View their challenge timetable.
Lastly, our tool gives Providers and Commissioners additional options to:
- View a Plan vs Actual vs Challenge graph and table.
- Search for a spell or patient, and see the patient spell history and spell challenge status (if challenged).
- Manage their user profile and change their login password.
- View a challenging library that defines the logic of each challenge.
- Upload their SLAM reports to a SLAM repository.
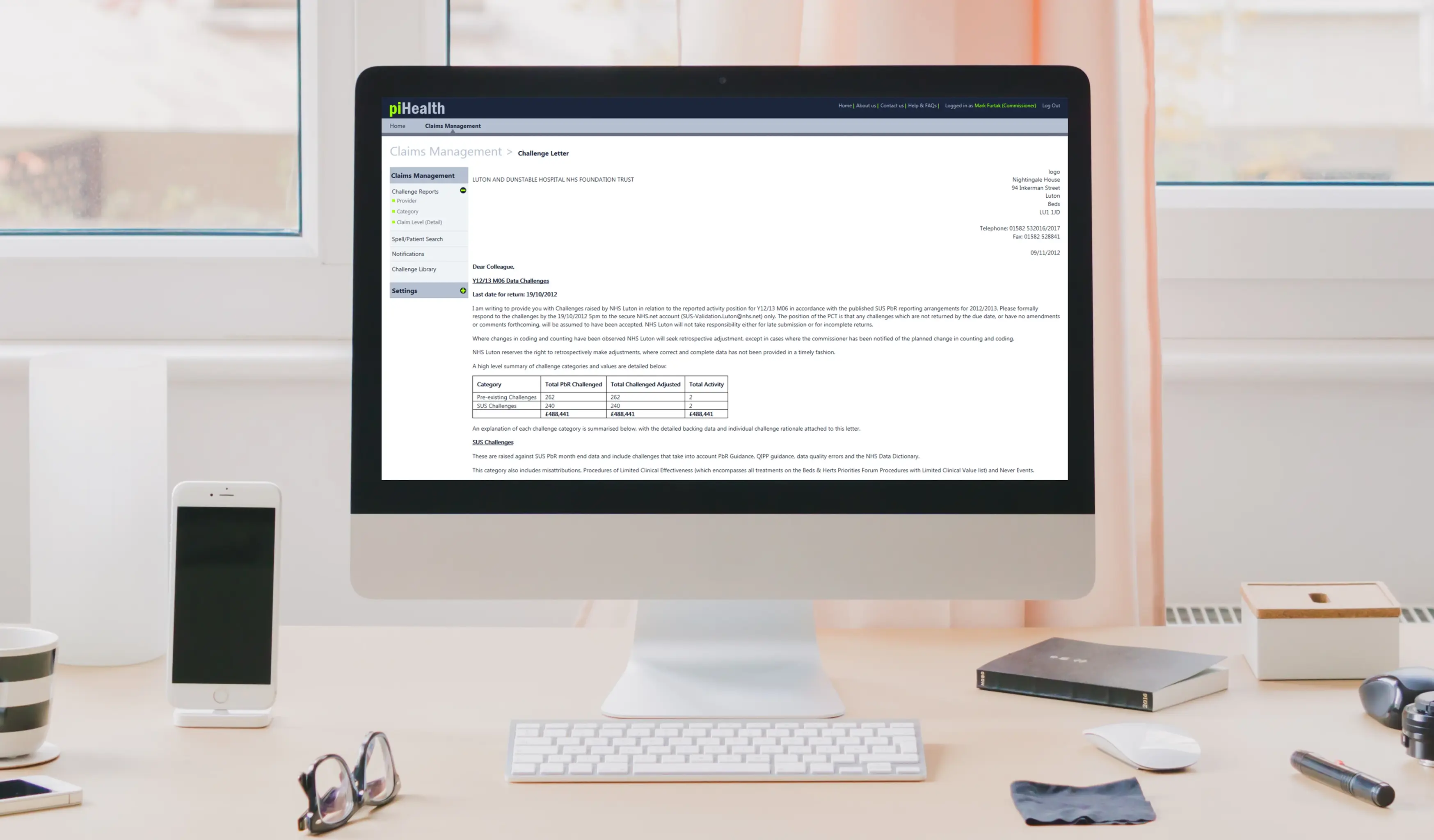
Outcome
Our invoice validation tool has successfully transformed Pulse Informatics’ idea and ambition into a reality. The tool supports NHS commissioners to create a more cost-effective service by:
- Guaranteeing that service providers are paid correctly and appropriately for a patient’s treatment
- Confirming that the correct patient received the treatment as specified and that the right provider and commissioner have been identified
- Allowing NHS services to be planned, commissioned, managed, and subjected to financial control
- Supporting commissioners to carry out their duty of fiscal scrutiny in an easier and more accurate way
- Enabling invoices to be challenged and issues to be resolved on a centralised platform
We, therefore, consider our partnership with Pulse Informatics to be a success. Ultimately, this tool can be used to support the NHS to navigate the many and multifaceted pressures it faces and helps to improve the health value for each patient.
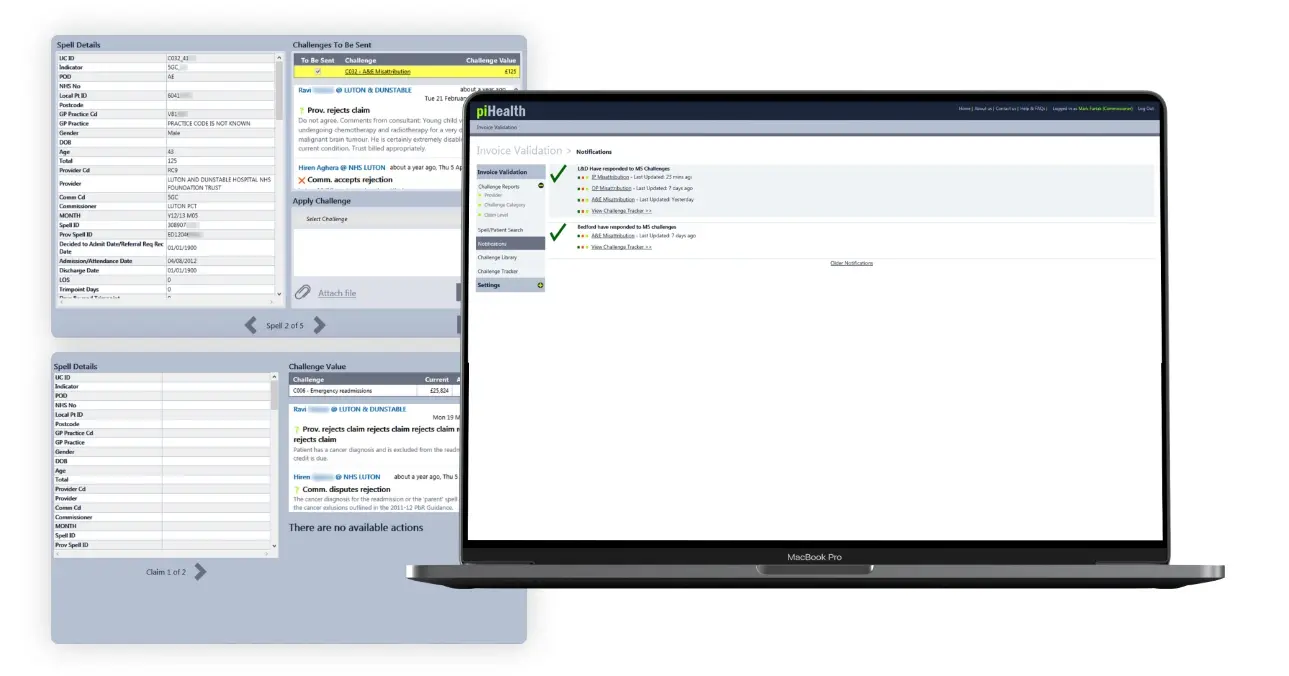
Project facts
- Team – Developers 2 (Fullstack dev 2), PM 1
- Project management – Waterfall
- Technology – .NET Framework